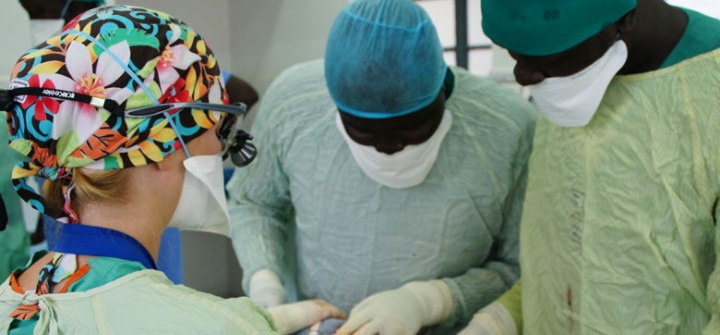
Surgery is Central
Imagine that your child has been injured and desperately needs surgery, but instead of getting immediate treatment, you’re hunting around the market for surgical supplies. Or driving from clinic to clinic, trying—in vain—to find someone to help your child.
Those are the kinds of stories that parents in West Africa shared with Fizan Abdullah, MD, PhD, chair of the Global Alliance for Surgical, Obstetric, Trauma, and Anesthesia Care (G4 Alliance) and vice-chair of the Department of Surgery at Lurie Children’s Hospital of Chicago. And they are not unusual: 5 billion people around the world do not have access to safe surgical care and anesthesia. The numbers are stark:
- In 2010, an estimated 16.9 million people died due to untreated surgical conditions
- Surgical conditions represent 28-32% of the global burden of disease
- Globally, the poorest 1/3 receives only 6% of all surgical procedures
- 81 million people face financial ruin from payments for surgical care
It all adds up to a need for urgent action, which a panel assembled by the G4 Alliance articulated at a briefing on Capitol Hill this week. The movement emphasizes that surgical needs are not just another issue elbowing for attention. Rather, surgical care is foundational to many other needs, from maternal health to non-communicable diseases.
Consider, for example, that 60% of cancer patients require surgery, or that timely detection and obstetric surgery could prevent up to 90% of maternal deaths. That’s why Mark G. Shrime, MD, MPH, PHD, FACS, research director of the Program in Global Surgery and Social Change at Harvard Medical School and of the Lancet Commission on Global Surgery, said, “We’re not talking about surgery instead of maternal health, or the other problems we’ve committed to. We’re talking about surgery because of maternal health … because we as a country have invested a lot in global health and we’re not going to get a return on our investment that we should be getting without scaling up surgery systems.”
Scaling up will require a lot of investment. In terms of clinical infrastructure, for example, the needs include oxygen, safe water and a stable electrical supply, along with biomedical engineering and technical training. Asha Varghese, director of Global Health for the GE Foundation, described how less than 30% of ORs in Kenya, Tanzania and Uganda have dependable water and electricity, and in low-resource hospitals, 40-70% of medical equipment is out of use at any given time. Furthermore, fewer than 1 in 3 facilities in East Africa employ staff capable of passing a basic test on proper sterilization procedures, and fewer than 50% of hospitals in Africa have effective infection control processes. These shortcomings all contribute to maternal mortality in the developing world, Varghese said—and addressing them is central to achieving the goal of ending preventable maternal and child deaths.
Surgeons, anesthesiologists, and nurses are key to that effort as well—but training and retention efforts are not keeping pace with needs. “The ILO (International Labor Organization) estimates a current deficit of at least 10.3 million health workers needed to provide essential health services worldwide, including at least 7 million in rural and remote areas,” according to Vince Blaser, acting director of the Frontline Health Workers Coalition. To support training and development of the health workforce, especially in the least-developed countries, he pointed to a bipartisan resolution on frontline health workers currently before the US Congress, H Res 419, as a great starting point for conversations.
Abdullah offered some more specifics for a call to action for the US government to set policy and mobilize resources to close the surgery gap, including:
- Advocate for integration of surgical care as part of US government foreign assistance funding and programs.
- Join the Congressional Global Health caucus and stay informed about global surgical care.
- Support coordinated collection of surgical care data (operative case log, access, quality, affordability) and support integrated health system platforms and global standards for surgical delivery, quality and safety and skilled surgical and anesthesia workforce.
Improving access to surgery will require investments in everything from clinical infrastructure to human resources, but the economic benefits are as clear as the positive effects for other health goals. As Thomas Novotny, MD, MPH, deputy assistant secretary for health of the US Department of Health and Human Services, noted, “The cost of increasing surgical capacity is estimated at $350 billion. The cost of not investing in essential surgical care and anesthesia: $12.3 trillion.”
Join the thousands of subscribers who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: Subscribe to GHN
© 2011 Samuel Boland, Courtesy of Photoshare. In Juba, South Sudan, a surgeon working with Massachusetts General Hospital's Division of Global Health and Human Rights assists South Sudanese surgeons with an amputation of a young girl's malignant tumor.