Cutting Through the Political Declaration on Universal Health Coverage
When the UN convenes its High-Level Meeting next week on universal health coverage, increased access to surgery not only needs to be a top priority for political rhetoric but for genuine commitment.
“No country can achieve universal health coverage unless its people have access to safe, timely, and affordable surgical services,” WHO Director-General Tedros Adhanom Ghebreyesus, said earlier this year in remarks to the global surgery community in Dubai. “9 of the 13 targets of Sustainable Development Goal 3 will never be achieved without improved surgical care, and yet globally, 5 billion people … lack that access.”
Just 4 years ago, the World Health Assembly recognized this reality, unanimously adopting Resolution WHA68.15: “Strengthening emergency and essential surgical care and anesthesia as a component of universal health coverage”—a historic document, yet one that attracted limited political commitment in the years that followed.
At odds with the political ambivalence, over 18 million people die annually from lack of access to emergency and essential surgical care, and one-third of the global burden of disease calls for surgical treatment.
The need to holistically strengthen health systems to become viable surgical ecosystems looms urgently.
On September 23, at the UN High-Level Meeting on UHC at the 74th UN General Assembly in New York, the adoption of the Political Declaration on UHC will be a central focus. The Declaration supposedly symbolizes further political commitment to the development agenda and the road to health for all by 2030. Nevertheless, civil society understandably fears that the HLM-UHC will be another “business-as-usual global health event.” The Political Declaration has undergone major changes, morphing from a powerful initial draft holding governments accountable in January to a more ambiguous, uncommitted final draft in August.
While governments initially committed to spending 5% of their GDP on health, they now simply adhere to the 1% increase proposed by the WHO and the Declaration. Further, no governments express specific national UHC commitments ahead of the HLM, preventing civil society interaction. Additionally, limited private sector regulation impedes the potential to optimize public-private partnerships for improved accountability and impact.
Billions lack access to life-saving or life-changing surgical, obstetric, and anesthesia care. Every year, 81 million individuals are pushed (further) into poverty to receive surgical care, and many millions more fail to seek services due to fear of financial ruin. Since WHA68.15 passed, only a handful of countries have developed National Surgical, Obstetric, and Anesthesia Plans, known as NSOAPs, though that process is underway in dozens more. LMICs only need to invest a minimal amount to ensure timely access to safe and affordable surgical, obstetric, and anesthesia care: Rwanda (0.13% of GDP per capita needed), Tanzania (0.16%), Zambia (0.24%), and Nigeria (0.87%) based on their own projected costs. On the flipside, failing to invest in surgical services may impede LMICs’ socioeconomic growth by up to 2% by 2030.
During last May’s WHA, Tedros updated the global community on progress on the 2030 sustainable development goals. Recognizing the growing NSOAP movement around the world, he raised the need for governments to continue to support systems-wide interventions as a cross-cutting horizontal approach, as opposed to traditional vertical disease silos. Others have set off alarm bells, too; the opening words of WHA72 by Richard Horton, The Lancet’s editor-in-chief, were full of emotion and memorable. Just a few weeks prior, he was treated and operated on for metastatic cancer, free at the point of care. He realized he was lucky, but that millions are not so fortunate.
At next week’s UN General Assembly, the million-dollar question remains: Will the world be able to achieve UHC by 2030—just over 10 years away? Cross-cutting and comprehensive health systems strengthened with emergency and essential surgical services—aligned with primary health care interventions and backed up by budgets—will prove key in truly bringing health for all to all.
Richard Horton was able to obtain treatment and go on to speak up. If countries do not make the political and financial commitment needed to ensure broader access, millions will never have that same opportunity.
Dominique Vervoort, MD, is a Belgian physician and MPH/MBA student at the Johns Hopkins Bloomberg School of Public Health and Johns Hopkins Carey Business School. He previously completed the Paul Farmer Global Surgery Fellowship at Harvard Medical School.
Join the tens of thousands of subscribers who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: http://www.globalhealthnow.org/subscribe.html
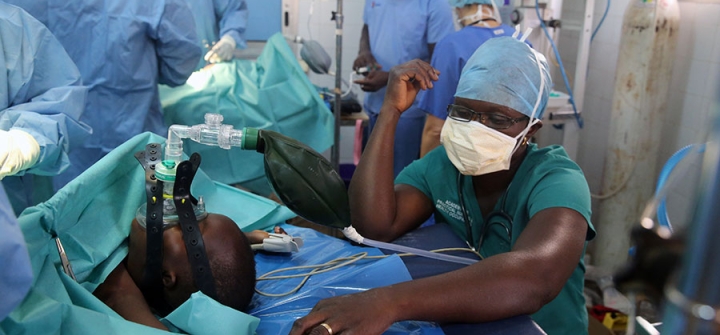
In the operating theater at Sotouboua hospital in Togo, Africa. Image: BSIP/Universal Images Group via Getty