Clade X: A Mock, Yet Entirely Plausible, Pandemic
WASHINGTON, DC—In mid-May, the US National Security Advisor assembled a team of top advisors to discuss the mysterious illness emerging in Germany and Venezuela, with hundreds of cases and dozens of deaths since mid-April.
Patients, including US military members, were showing up at the hospital in Landstuhl with fever, cough, and confusion. Some patients were ending up on respirators; others fell into comas.
Initially, it looked like viral encephalitis. But it soon became clear this virus was something new—and lethal. It had the ability to be transmitted from person to person through the air, a 5-7 day incubation period, and a high fatality rate.
At this point, officials had no reason to believe the virus was anything other than a naturally occurring virus.
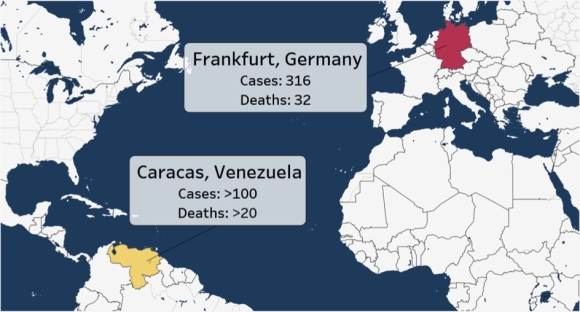
May 1, 2018: Clade X Global Cases
By May 1, the virus had spread to Venezuela. And while Germany’s health system moved fast to isolate the sick and track exposures, the authorities in Venezuela reacted much differently, denying the outbreak. Hundreds of people soon swamped ERs. The US Coast Guard reported seeing boats of sick refugees from Venezuela approaching Puerto Rico.
By May 2, a culprit had been identified: parainfluenza. Human Parainfluenza Viruses, as the CDC explains, are different than influenza viruses, although they also can cause respiratory infections—and the flu vaccine does not protect against HPIV infections.
The mystery virus—with no known antivirals, no licensed vaccines against it, and pandemic potential—got a name: Clade X.
Thankfully, Clade X is not real, and this was a mock pandemic—an exercise hosted by the Johns Hopkins Center for Health Security last week.
But don’t get too comfortable; the underlying storyline is all too plausible.
The advisors, a distinguished cast of ex-officials with plenty of real-world experience in their adopted roles, grappled with critical dilemmas—while intermittent mock newscasts delivered steadily worsening news about the outbreak.
The simulation aimed to spur US officials and researchers to think through challenging scenarios and questions before the next health emergency strikes. For instance, should the US cave to public pressure and issue travel bans and quarantines when a workable vaccine is likely one year away, no rapid diagnostic test exists, and other countries shut down travel?
The assembled experts quickly mapped out the case against travel bans. Julie Gerberding, MD, MPH, playing the role of the CDC director (a role she held in real life from 2002-2009), pointed out that Frankfurt is a major airport hub, so banning just one leg of the journey wouldn’t work. Travel bans, she explained, are simply “…not effective, impractical and potentially harmful.”
The White House National Security Advisor, played by Tom Inglesby, MD, director of the Center for Health Security, pushed the Council to consider whether there could be any circumstances under which travel would be banned? And, if not, he asked, how should that be explained to Americans, given bans by other countries? The discussion underscored the importance of education and communication surrounding sensitive issues that might seem counterintuitive to people outside the public health community.
Turning to the situation unfolding in Venezuela, the Cabinet considered another question: Should the US send a substantial medical response to Venezuela, though their security and access to health care would be tenuous?
That question stirred lively debate over the security of US health workers versus the US’s interests in offering support to a county in need and blocking the disease’s spread. Reprising his former role as the Senate Majority, Tom Daschle summed up the case for getting involved: “If you don’t visit a bad neighborhood, it will visit you if we don’t have an urgent plan to contain.”
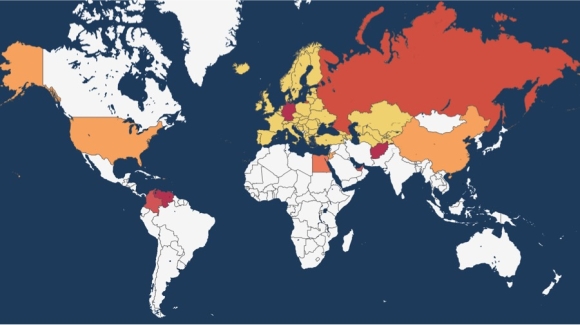
Spread of Clade X as of June 1, 2018
By the next mock meeting, on June 1, 2018, there was a large Clade X outbreak in Afghanistan. It also hit a US college dorm in Massachusetts, and soon after, Bethesda, Maryland. Lab analysis showed that Clade X had been deliberately engineered; bioterrorists, the Council learned, had inserted genes for neurologic virulence of Nipah into the parainfluenza genome.
The FBI learned that a splinter group of an international organization focused on overpopulation, A Brighter Dawn, was behind the attacks; one member of the group, a parainfluenza researcher from the US, could not be located.
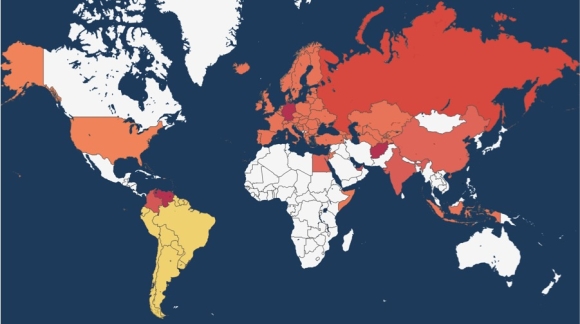
Spread of Clade X as of June 17, 2018
With the knowledge that terrorism was behind the outbreaks, a severe pandemic looked possible by mid-June 2018. With no preexisting immunity, modeling suggested a possibility of 0.5-2 million US deaths over the next year and >50 million globally.
By June 17, Jordan was fighting a severe Clade X outbreak, and terrorists from the Syrian Republic and Iraq exploited the government’s weakened state to take over the city of Mafraq. Jordan and Israel requested US assistance to stabilize the situation, leading the Council was grappling with questions like “Should we deploy military personnel to assist Jordan?” and “What should we do about hospitals that refuse to accept Clade X patients?”
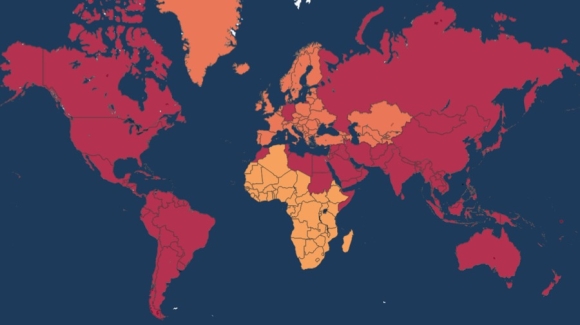
Spread of Clade X as of September 15, 2018
The US ended up deploying a brigade of about 4,500 people to Jordan. And by September, 5 months after onset of the first illness, many of those US troops had died from Clade X.
In the US, the virus had spread to nearly half of US states, with nearly 60,000 cases and 3,500 deaths—overwhelming hospitals and straining the supply of surgical masks and respirators. The CDC began encouraging telework and social distancing—including school closures and cancelations of public gatherings. Multiple states deployed National Guard to provide security at pharmacies and hospitals.
Globally, the probable and confirmed cases totaled over 8.7 million, with over 3.1 million deaths. Amid high transmission in megacities, some countries deployed military to keep order and secure borders. Widespread looting in some countries led to violent government crackdowns. A catastrophic outcome seemed likely unless a vaccine could be deployed soon.
One American-made vaccine candidate looked promising. With estimates indicating that enough vaccine could be produced for 80% of the US population in 6-9 months, the National Security Council advisors began to consider how to best allocate limited vaccine to Americans. Should they prioritize those with value to others (e.g., health care workers, scientists working on the vaccine, the military, and key government officials)? Or those most likely to benefit—like children and pregnant women. Or, should they opt for a lottery, giving everyone an equal chance?
“The harder question,” said the Secretary of Defense, played by Jim Talent, a former US senator, “is do we share with those parts of the world that are not capable of producing a vaccine?” Unfortunately, that would add up to most of the world.
That spurred advice from the CIA Director, played by Jeffrey Smith, former CIA general counsel: “This will come to an end … and how we behave as a country will determine how other people judge us in other parts of the world. Somehow we have to keep alive the hope that we can help other countries.”
By the end of the exercise, the much-anticipated first vaccine flopped, and although another vaccine candidate emerged and Clade X did eventually burn out, it brought the entire world to its knees first.
If you missed it, but you want to see how experienced leaders grappled with these questions, you’re in luck: You can watch the livestream here. And, over the coming weeks, the Center for Health Security will be pulling together the advice developed in the meeting and translating it into policy recommendations.
Join the tens of thousands of subscribers in more than 100 countries who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: http://www.globalhealthnow.org/subscribe.html




