A 2-Front Battle: COVID-19 Must Reinvigorate the Fight Against TB
As the COVID-19 scourge intensifies, it may be weakening our battle against tuberculosis—but pooling resources could boost the fight against both diseases.
While human and financial TB resources have been diverted to fight the pandemic, new TB case notifications have dropped by up to 75% in some countries, according to a Global Fund report published in September. In addition, TB service disruptions could lead to an additional 1.4 million deaths through 2025.
Public health crises have historically been a catalyst for progress. The 1918 influenza pandemic led to many new or revamped national public health ministries. The first global effort to contain infectious disease, the 1851 International Sanitary Conference in Paris, addressed the cholera epidemic that ravaged Europe and the Middle East.
With the right efforts and investment, the COVID-19 response could double as the impetus for a truly sustainable fight against TB.
Here’s how:
TB programs must be fully funded: The 2018 funding pot for TB research—$906 million—must be doubled to meet annual needs through 2022. In 2020, some $6.5 billion is available globally for TB prevention, diagnosis, and treatment efforts—just 50% of the target per year through 2022. While efforts to defeat the coronavirus drain coffers meant to fight TB, forecasters are predicting the worst global recession since WWII. Funding now earmarked for COVID-19 should instead be used to address both disease threats, creating a more cost-efficient approach to surveillance and diagnosis.
Optimize available resources: Governments can tap the expertise of national TB programs, TB control systems, and communities to design an integrated response that makes use of the infrastructure and workforce for both COVID-19 and TB.
- TB laboratory networks and specimen transport systems can be used for COVID-19 diagnosis and surveillance.
- Point-of-care rapid molecular tests like Xpert and TrueNat can be used to diagnose both TB and COVID-19.
- Contact tracing networks established during the pandemic can expand to include TB.
- Experienced TB control staff in the field can provide much-needed capacity in active case finding and contact tracing for COVID-19.
Strengthening community surveillance, which can cover both diseases, can reach presumptive TB cases early at home—key as some people may avoid health facilities due to fear of COVID-19 and stigma. After all, TB and COVID-19 are both infectious diseases attacking primarily the lungs, with similar symptoms (cough, fever, and difficulty breathing) that could indicate either disease.
Fortify national leadership with multisectoral collaboration: It is imperative to have sustainable leadership capable of handling public health emergencies. But this isn’t achieved overnight, nor in a vacuum, in countries that are still establishing public health governance.
My organization, Management Sciences for Health, is working via a USAID-funded health systems strengthening program that helps low- and middle-income countries increase domestic funding and use resources efficiently to finance TB care and prevention, while building in-country technical and managerial competence and leadership. It is essential to improve in-country policy and legal frameworks that enable inclusive TB governance for nongovernment actors, like the private sector, civil society, professional associations, communities, and people affected by TB.
Local outreach is also key, and health care workers and local organizations promoting trust, behavioral change, and advocacy are vital in TB control. A number of countries have used this approach to great effect in fighting COVID-19. In South Africa, for example, NGOs have led community action networks to help feed those affected by the pandemic. We need this kind of creativity to jumpstart efforts to end TB.
World leaders have committed to treating 40 million people for TB by 2022 and to providing preventive treatment for 30 million more. Meanwhile, the COVID-19 death toll has passed 1.5 million people. The scourge of both diseases demands informed, inclusive, and empowered public health leadership.
We must use this mandate to rethink how we fight TB. It will strengthen our position now and for decades to come, saving millions of lives.
Ersin Topcuoglu, MD, MPH is the Director of the USAID-funded Health Systems for Tuberculosis Project at Management Sciences for Health, a nonprofit global health organization.
For the latest, most reliable COVID-19 insights from some of the world’s most respected global health experts, see Global Health NOW’s COVID-19 Expert Reality Check.
Join the 50,000+ subscribers in 170+ countries who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: https://www.globalhealthnow.org/subscribe
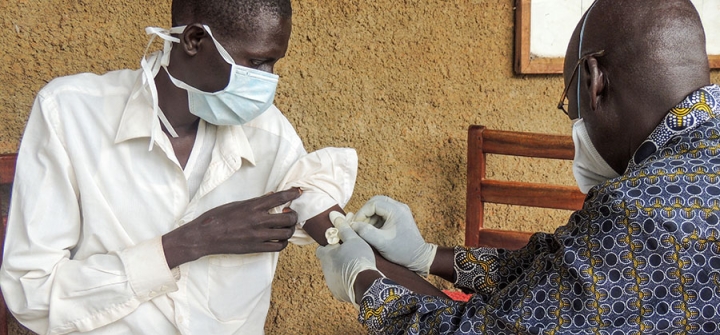
A health worker takes a blood sample from an XDR-TB patient at Kitgum Hospital in northern Uganda Image: Diana Tumuhairwe, Management Sciences for Health