After Years of War, the Fight for Health
Over 26 years of civil war in Somaliland completely decimated its health services. In the chaos, many health care professionals were either killed or fled the country, more than half a million people lost their lives, and a further million became refugees. Civilians were subjected to genocide and mass killings, and health facilities were razed.
But in 1991 Somalilanders claimed independence from Somalia and focused on rebuilding their lives—and health services—ever since. And although some health facilities have been rebuilt, or built from new, like the Edna Adan Hospital in Hargeisa, Somaliland continues to suffer from a severe shortage of trained health professionals and appropriate medical equipment.
In response to this need, a global collaboration in the shape of a public-private partnership (PPP) emerged to improve the quality, safety, and access to surgical care in this region.
By definition, access to safe surgical care means access to safe anesthesia—which an estimated 5 billion people around the world do not have. SANSOM, or Safe Anaesthesia for Somaliland, brought together 5 international organizations—a charity, a foundation, 2 NGOs and a commercial business—to make a small but meaningful dent in this statistic.
Building on 2 years of training for nurse anesthetists by Mark Newton, MD and his colleagues at AIC Kijabe Hospital, Kenya, a January 2017 conference at the Edna Adan Hospital in Hargeisa gathered students from across Somaliland for further training, and to consolidate and strengthen their knowledge.
Now, there are more than 30 well trained nurse anesthetists working in Somaliland. And although there is still not a single consultant anesthesiologist in the country, SANSOM ensured that all 6 regions of Somaliland now have a provision for skilled anesthesia care in the shape of nurse anesthetists.
A parallel initiative driven by Diamedica UK Ltd, SANSOM aimed to train and equip newly qualified anesthesia providers with appropriate equipment, such as portable anesthesia machines, oxygen concentrators, pulse oximeters, and more.
Despite well-intentioned donations from the west, suitable medical equipment for low-resource settings can be very hard to come by. Indeed, western donations can often become abandoned ‘apparatus graveyards’ of machines. That’s because this equipment can’t function in a remote field hospital where there may be an erratic electricity supply, unavailability of compressed oxygen, an absence of biomedical engineers familiar with the equipment, or no access to spare parts for repairs.
Crucially, the portable anesthetic machines donated for SANSOM—accompanied by oxygen concentrators to address oxygen shortage problems—were designed for optimum functionality in low-resource environments.
Medical staff in Somaliland are as conscious as anyone else in the world of the challenges set by the UN’s Sustainable Development Goals—in particular SDG3, on Health and Well-Being. They also aspire to Universal Health Coverage, but here, with one of the highest infant mortality rates in the world, one in 7 children won’t reach their fifth birthday. Their mothers face a lifetime risk of one maternal death for every 10 women.
Since surgery can successfully treat conditions from cancer to obstructed labor, access to safe, timely and affordable surgical care and anesthesia is essential for these at-risk women. Reports from the hospitals that participated in SANSOM confirm improvements have already been made in reducing both infant and maternal mortality. What’s more, for the first time in the country’s history this data is being recorded on tablets donated as part of the project.
Initial assessments following SANSOM show that it is possible to make a huge difference on a comparatively small budget, fueling optimism in the participating medical staff. Keys to success, according to SANSOM, included bringing an appropriate innovation to the development table—in this case, a portable anesthesia machine and oxygen concentrator exclusively designed for challenging environments.
The project also adopted a community-centric approach, using a sustainable education model to counter ‘brain drain’ with an emphasis on homespun training and follow-up opportunities. The donated equipment also gave newly trained nurse anesthetists a way to practice their new skills, and the potential for rewarding medical careers at home.
SANSOM’s lessons showed that practical solutions aimed at a critical need—the lack of surgical access in Somaliland—can save lives, and provide a model to help close a persistent health disparity between the West and low-income countries.
Andrea Charters is the Communications Executive for Diamedica UK Ltd, a journalist, former newspaper sub editor and recently the editor of two international medical journals. She writes extensively on global health matters and directed an award-winning documentary film on this subject, SANSOM – Partnerships for Progress, in Somaliland.
Join the tens of thousands of subscribers who rely on Global Health NOW summaries and exclusive articles for the latest public health news. Sign up for our free weekday enewsletter, and please share the link with friends and colleagues: http://www.globalhealthnow.org/subscribe.html
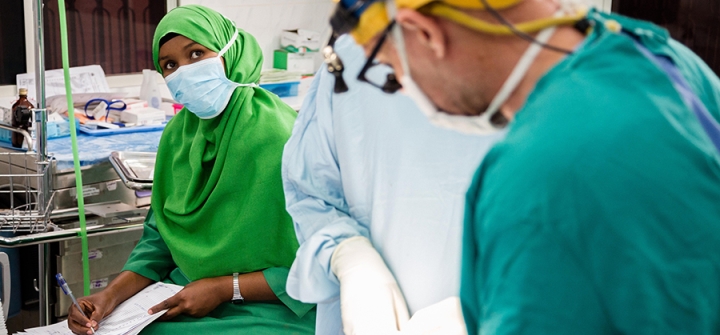
Hamda Mohamed Omar (left), a nurse anesthetist/trainer from Edna Adan hospital in Hargeisa, at work with a visiting surgeon. Photo by Tim Bekir.